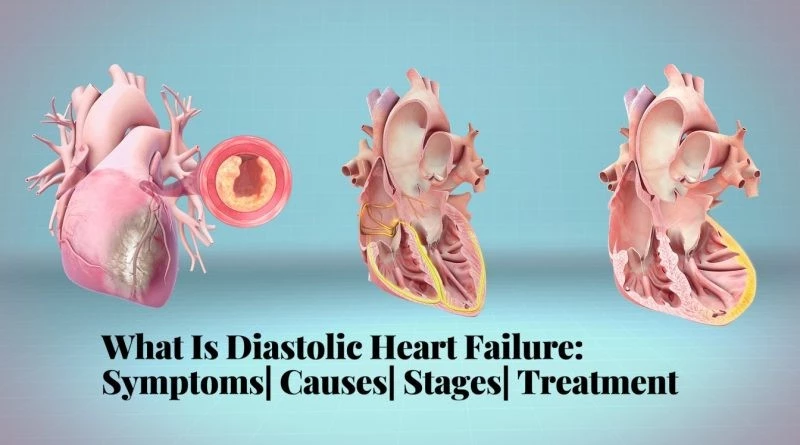
What Is Diastolic Heart Failure: Symptoms| Causes| Stages| Treatment
If you have diastolic heart failure, your left ventricle has become tighter than normal because of this, your heart cannot relax the way it should. The heart when it pumps, cannot fill with blood as it is supposed to. Because there is less blood in the ventricles, less blood is pumped into your body.
Table of Contents
Symptoms of Diastolic Heart Failure
Various Signs and symptoms of diastolic heart failure can range from mild to severe, and may incorporate-
- Waking up at night with shortness of breath
- Shortness of breath or difficulty in breathing during exercise or lying flat
- Cough or wheezing, sometimes even with white or pink phlegm
- Difficulty in concentrating
- Tiredness or weakness
- Fatigue
- Fluid retention causes swelling of the ankles, feet, legs, or abdomen.
- Loss of appetite and nausea
- Dizziness, confusion
- Rapid or irregular heartbeat
- Sudden weight gain
Causes of Diastolic Heart Failure
As we grow older, our heart and blood vessels become less elastic. This increases their chances of hardening/stiffening. Therefore diastolic heart failure is more common as people get older. Apart from normal aging, the most common reasons are:
High Blood Pressure- If you have this, your heart has to work harder to pump more blood into your body. Thanks to that extra work, your heart muscle can become thick or large, and it eventually becomes stiff.
Diabetes- The disease can make your heart wall thick. Which eventually makes it stiffen.
Coronary artery disease– The amount of blood flowing to your heart muscle is blocked or less than normal.
Obesity or Inactivity- With obesity or inactivity, your heart has to work harder to pump blood.
Kidney Disease- Kidney disease can cause heart failure.
Diagnosis of Diastolic Heart Failure
To find and figure if you have heart failure, your doctor will examine you and ask about your medical history, and do some tests. Those tests may incorporate-
Blood tests- Blood tests check the levels and amount of certain fats, cholesterol, sugars, and proteins in the blood that may indicate/show a heart condition.
Chest X-ray- This is a general imaging test of the lung, heart, and aorta.
Echocardiogram- This ultrasound examination utilizes sound waves to take moving pictures of the heart’s chambers and valves.
Electrocardiogram (EKG)- This test measures the heart’s electrical activity and can help determine whether parts of the heart are enlarged, overworked, or damaged. The electrical currents of the heart are detected by 12 to 15 electrodes that are connected via a sticky tape sticking to the hands, feet, and chest.
Heart catheterization- Cardiac catheterization (cardiac cath or heart cath) is a procedure to check and know how well your heart is working. A thin, hollow tube called a catheter is inserted into a large blood vessel that leads to your heart.
Stress test- This test is done during exercise. If a person cannot exercise, medication is given to increase the heart rate. Used with an EKG, the test may show changes in heart rate, rhythm, or electrical activity as well as blood pressure. Exercise makes the heart work harder and beats faster during the examination of the heart. الرهان في سباق الخيل
Diastolic Heart Failure Stages
Stage1- Physical activity causes no problems to the person, such as fatigue, palpitations, or difficulty breathing.
Stage 2- There are some limitations in a person’s physical activity. The person feels comfortable while resting. A person’s normal physical activity makes them tired, gives them palpitations, or causes shortness of breath.
Stage 3- There are substantial limitations in the physical activity of the person. The person feels comfortable while resting. Physical activities less difficult than daily tasks cause fatigue, palpitations, or shortness of breath. ربح الاموال
Stage 4- A person cannot do any kind of activity without any trouble and discomfort. When resting, a person shows signs of heart failure. If the person tries any type of physical activity, he feels more uncomfortable.
Diastolic Heart Failure Treatment
Medications
Medications might be recommended to treat or lessen symptoms of diastolic heart failure. This diastolic heart failure treatment include-
- Angiotensin-Converting Enzyme Inhibitors (ACE Inhibitors) and Angiotensin Receptor Blockers (ARBs), which loosen up and relax veins to improve blood flow.
- Beta-blockers, which can diminish blood pressure and moderate a rapid heart rhythm.
- Calcium-channel blockers and long-acting nitrates loosen up and relax blood vessels, particularly those that feed the heart muscle.
- Diuretics decrease your body’s liquid substance by promoting pee.
- Vasodilators to open blood vessels if you can’t tolerate ACE inhibitors or ARBs.
- Surgery and Other Procedures
Diastolic heart failure surgery
If medications are not effective, your doctor may suggest surgery which s basically a form of This diastolic heart failure treatment it includes-
- Angioplasty- to open a blocked artery or surgery to repair a heart valve.
- Heart valve repair- Repair or replacement of heart valves can help to fix or correct diastolic heart failure.
Lifestyle Changes that can Prevent Diastolic Heart Failure
Although you cannot prevent all types of diastolic heart failure, you can take steps to reduce your risk for illnesses or conditions that may exacerbate or complicate the condition.
Try to be active- Moderate exercise helps circulation and decreases stress on your heart muscle.
Regular checkups- If you experience new or changing manifestations or side effects from medications, consult your doctor.
Get a healthy diet to make your heart happy– Limit sugar, saturated fat, cholesterol, and salt, and eat a lot of natural products, fruits, vegetables, whole grains, and low-fat dairy items.
Maintain a solid weight- Losing weight and keeping a sound weight puts less weight and stress on the heart.
Decrease your liquor intake- In some cases, you may have to stop drinking alcohol altogether. If you can drink, keep your intake low.
Quit smoking- Because Smoking damages blood vessels raises blood pressure, reduces the amount of oxygen in the blood, and makes your heart beat faster.
Take your medications as prescribed- If you have been prescribed medicine for diastolic heart failure or a causative condition, be sure to take it as prescribed.
Systolic vs Diastolic Heart Failure
Diastolic Heart Failure
Diastolic heart failure occurs when your left ventricle can no longer rest between heartbeats because the tissues have hardened. When your heart cannot completely relax, it will not fill with blood again before the next beat.
Systolic vs Diastolic heart failure the difference is simply the Diastolic heart failure type is also called heart failure with preserved ejection fraction (HFpEF). In this type, your doctor can do an imaging test on your heart and determine if your EF looks fine. Your doctor will then should consider if you either have any other heart failure symptoms and if there is evidence that your heart is not functioning properly. If all those criteria are met, you may be diagnosed with diastolic heart failure.
This kind of heart failure often affects older women. It often accompanies other types of heart disease and other non-heart conditions like cancer and lung disease.
Systolic Heart Failure
Systolic vs Diastolic heart failure the difference is simply the Systolic heart failure occurs when the left ventricle of your heart does not completely contract. This means that your heart will not pump sufficiently to move your blood throughout your body in an efficient manner. It is also called heart failure with low ejection fraction (HFrEF).
Ejection Fraction (EF) is a measure of how much blood is released each time the heart ventricle is pumped. The more the heart pumps, the healthier it is.
After performing an imaging test such as an echocardiogram, the doctor will tell you your EF as a percentage. EF between 50 and 70 percent is considered normal. (Even if your EF is normal, it is still possible to have other types of heart failure.) If your EF is less than 40 percent, then you have reduced ejection fraction or systolic heart failure.
FAQs Related to Diastolic Heart Failure
What happens when there is diastolic heart failure?
If you have diastolic heart failure, your left ventricle has become tighter than normal. استراتيجية روليت Because of this, your heart may not rest the way it should. When it pumps, it cannot fill with blood as it is supposed to. Because there is less blood in the ventricles, less blood is pumped into your body.
What is the life expectancy with diastolic heart failure?
Diastolic heart failure (HF), as defined by the symptoms and indications of HF, preserved ejection fraction, and abnormal diastolic function is approximated to occur in half of all patients presenting with HF. Patients with preserved ejection fraction are older and more often female. The underlying etiology of HF varies, hypertension is more often usual in the patients with preserved ejection fraction, and ischemic heart disease predominates in those with lower ejection fraction.
Diastolic HF is related to a higher mortality rate than that of HF with depressed ejection fraction with a minimum five-year survival rate after the first episode of 43% and a higher mortality rate than the rest general population. Also after significant disease burden, clinical and biological disease-related factors in diastolic HF remains less understood. There is also limited data from well-designed studies considering effective treatment strategies for this group of patients.
The patients with diastolic HF aging, male gender, non-Caucasian ethnicity, history of coronary artery disease, and atrial fibrillation are related to poor prognosis. Anemia and B-type natriuretic peptide are very important laboratory variables that predict mortality.
Diastolic dysfunction in exercise and its role for exercise capacity?
Diastolic dysfunction occurs more frequently in elderly subjects and patients with left ventricular hypertrophy, vascular disease, and diabetes mellitus. Patients with diastolic dysfunction display reduced exercise capacity and may suffer from congestive heart failure (CHF).
The presence of symptoms of CHF in the setting A normal systolic function is referred to as heart failure with normal ejection fraction (HFNEF) or, if evidence of a poor diastolic function, such as diastolic heart failure (DHF), is seen. Decreased exercise capacity in diastolic dysfunction results from several pathophysiological changes such as slow myocardial relaxation, reduced myocardial distensibility, elevated filling pressure, and reduced ventricular suction force.
These changes limit ventricular diastolic filling and increase cardiac output during exercise and give rise to pulmonary congestion. In healthy subjects, exercise training can increase diastolic function and exercise capacity and prevent the diastolic function from deteriorating during aging.
In patients with diastolic dysfunction, exercise capacity can be increased by exercise training and pharmacological treatment, whereas improvement in diastolic function may be seen only in some patients.
What are the signs your heart is quietly failing?
- Shortness of breath (dyspnea) when you exert yourself or if you lie down.
- Fatigue and weakness.
- Swelling (edema) in your feet, ankles, and feet.
- Fast or irregular heartbeat.
- Decreased ability to exercise.
- Constant cough or wheezing with white or pink blood-rich phlegm.
- Increased the need to urinate at night
What Is Diastolic Dysfunction?
Every time a healthy heart pumps oxygen-rich blood through the lungs to the rest of the body, it goes through two phases – a contraction or pumping phase (called systolic function) and a resting phase (called diastolic function).
When the heart muscles become stiffer which means that they cannot relax properly, leading to a condition called diastolic dysfunction. This flexibility prevents the heart’s ventricles from filling up entirely, causing the blood to back up in the organs. Diastolic dysfunction is an important cause of pulmonary hypertension (increased blood pressure in the lungs).
What is the number one cause of diastolic dysfunction?
The most common reason for this hardening/stiffening of the heart is old age. It is estimated that more than 50% of adults over the age of 70 have diastolic dysfunction.
- Other reasons may include-
- The high blood pressure
- Uncontrolled diabetes
- Kidney dysfunction
- Some cancers and genetic disorders, in normally rare cases
What is the life expectancy of someone with congestive heart failure?
Many people with heart failure can be overly optimistic when it comes to estimating how long they have left to live. A new study shows that nearly two-thirds of people with congestive heart failure shorten their remaining life expectancy by an average of 40%, compared to what is realistic based on their prognosis.
Heart failure, which occurs when the heart is too weak to pump enough blood to meet the needs of the body, causes 55,000 deaths each year, and indirectly in the U.S, it contributes to 230,000 more deaths annually.
Although treatment for congestive heart failure has improved recently, researchers say the prognosis for people with the disease is still bleak, with about 50% having an average life expectancy of fewer than five years. For people with advanced forms of heart failure, about 90% die within a year.
Can Weight Loss Reverse Mild Diastolic Dysfunction?
Yes, Obesity is related to diastolic dysfunction. A 12-week low-calorie diet with successful and dedicated weight loss can lower down your blood pressure and heart rate and partially normalize diastolic dysfunction.
What is the best diet for diastolic dysfunction?
According to research l-sodium, dash diet improves diastolic function and ventricular-artery coupling in hypertensive heart failure with preserved ejection fraction.
What is worse diastolic or systolic?
Over the years the research has found that both numbers are equally and accordingly important in checking heart health. However, most studies show a higher risk of stroke and heart disease related to higher systolic pressure than to higher diastolic pressure.
Can you have diastolic dysfunction without heart failure?
Diastolic dysfunction is referred to a kind of condition in which abnormalities in mechanical function are present during diastole. The abnormalities in diastolic function may occur in the presence or absence of the clinical syndrome of heart failure and with normal or abnormal systolic function.
How do you know if you have systolic or diastolic heart failure?
Systolic dysfunction can be easily assessed by assessment of global ejection fraction and regional wall motion. Diastolic dysfunction can be indirectly diagnosed through normal or near-normal ejection fraction and changes in mitral filling pattern in the context of LV failure.